Afghans face impossible choices in their struggle for medical care
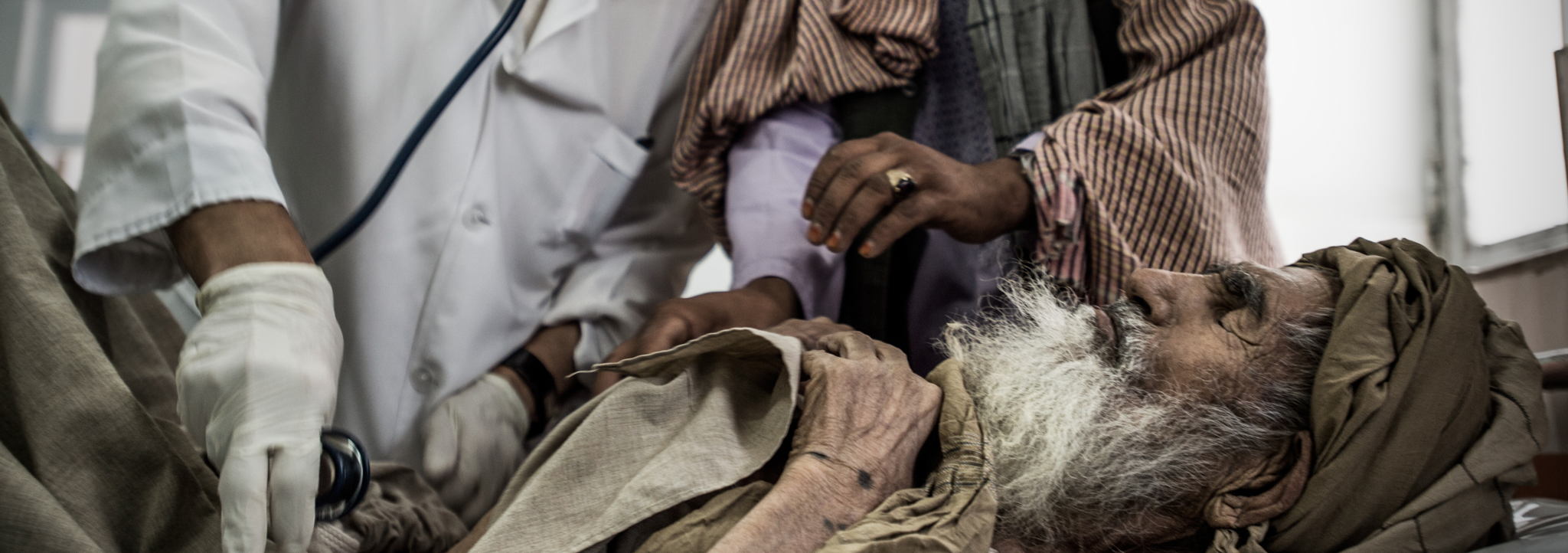
Despite decades of international aid and investment, Afghans still struggle to access basic and emergency medical care due to insecurity, distance, cost and the fact that many health facilities lack the staff and equipment they need, said Médecins Sans Frontières (MSF)/Doctors Without Borders today on the release of its report Reality Check: Afghanistan’s neglected healthcare crisis.
KEY FINDINGS:
Herat Regional Hospital:
41% of caretakers and patients surveyed stated that a family member, a friend or neighbour had died in the past two years due to lack of access to medical care.
Postponing medical care due to financial pressure is a dangerous coping strategy adopted by 89% of patients and caretakers surveyed; 43% stated they had postponed medical care more than three times over the past two years.
Boost Hospital
During the first six months of 2019, 44 per cent of the children who died within 24 hours of arriving at the paediatric intensive care unit in Boost hospital came too late and at a very advanced stage of illness.
Of 3680 measles cases treated in the first seven months of 2018, 48% were admitted to the isolation ward due to severe complications.
“We are scared to leave at night, so we always have to wait until daytime to go to the hospital,” said a patient’s caretaker in the maternity ward of Boost hospital. “With everyone in our family, when they are sick, we wait, even if the person is dying.”
The medical staff working in health facilities managed and supported by MSF regularly see the impact these delays have on patients’ health – delays that can mean the difference between life and death.
“One woman was in labour and she came for delivery. She was crying a lot, so we asked what happened. She said her sister-in-law, who was also pregnant, started bleeding the night before, around 11:30pm. There was fighting so they couldn’t leave the house. They waited until the fighting stopped and then they had to find a car to rent. By the time they found one her sister-in-law had died because of the bleeding. She said her contractions started because she became very afraid and she was crying a lot. Her husband took her to the hospital but then he had to return home to help his brother with the burial preparation.” - MSF Midwife, Maternity Ward, Boost Hospital, Lashkar Gah City, Helmand province
Poverty also has a significant impact on people’s access to medical care. Up to 89 per cent of patients and caretakers surveyed in Herat Regional Hospital said that they had postponed seeking medical care due to financial pressures. One parent explained that they had waited eight days to bring their malnourished baby for treatment while they scraped together the money to hire a car, eventually borrowing the funds from friends and relatives. Another simply said: “We cannot buy food for tonight. How can we pay for medicines and doctors?”
Over the last decade, civilian deaths and injuries due to armed conflict have nerarly doubled. Attacks on healthcare and disruption to the health system continue unabated. In 2018 Afghanistan ranked third in the world for the greatest number of attacks on healthcare, after Palestine and Syria, with 91 attacks reported by the WHO. Attacks continued in 2019 with 119 incidents reported as of the end of December.
MSF has worked in Afghanistan since 1980 and today runs six projects in six provinces: Kabul, Khost, Kandahar, Kunduz, Helmand and Herat. In 2018, MSF teams provided 411,700 outpatient consultations, assisted 74,600 births and undertook 6,890 major surgical interventions. MSF provides medical care free of charge. It relies solely on private funding for its work in Afghanistan and does not accept money from any government.
ENDS
.jpg)
.JPG)
.JPG)
.jpg)
.jpg)