Out of sight, but not out of mind: MSF’s COVID-19 response in care homes
Please find below a link to 4 pieces of b-roll from MSF's work in care homes across Italy, Spain and Belgium as well as two testimonies from our staff.
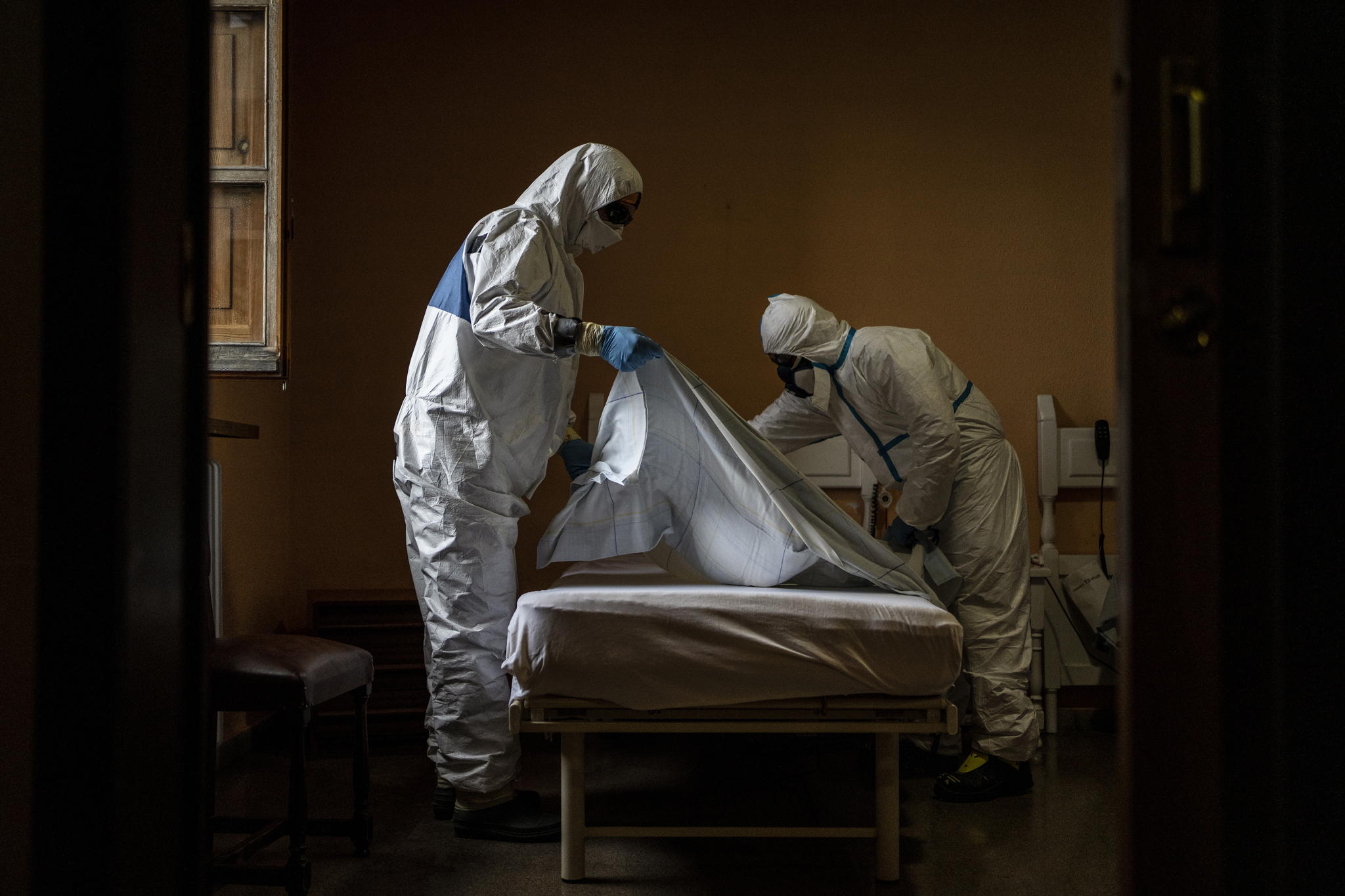
The COVID-19 pandemic cannot be said to have gone unnoticed as it crashes around the globe. But in the places it has hit hardest, the virus has made its way silently into all corners of society’s fabric. And it has taken one of the heaviest tolls in residential homes for elderly people, who need a very special level of care. In some care homes where MSF has assisted, as many as one in three residents have died – a mortality rate that would be shocking in any crisis.
Care homes are not hospitals and inevitably they lack the medical preparedness to face such a pandemic.
Acknowledging the complexity of this extraordinary situation, in MSF’s experience a variety of factors have led to the devastation caused by COVID-19 in these communities: the particular vulnerability of the residents, who are elderly and often frail and who need assistance with daily activities; little outbreak preparedness; little to no epidemiological surveillance; inadequate infection prevention and control; an increased workload for staff, coupled with decreased staff numbers due to people falling sick or self-isolating; and inadequate isolation of residents infected with COVID-19. MSF teams have invariably found staff who are trying their best, but who lack the resources and the specific training and technical support they need. All these factors have resulted in an insufficient quality of care, which has in turn influenced the increased number of COVID-19 patients.
The depth of psychological suffering of care home residents infected with COVID-19 is also enormous, as is the need for specific attention to palliative care and ways to allow human interaction between families and sick residents in the last days of life. “Too many people have been dying alone, frightened and in a terrible state,” says Dr Ximena di Lollo, who is coordinating MSF’s COVID-19 response in care homes in Spain and Portugal. “People have been cut off from their families and have faced the end of their lives with no support and barely any human contact. That is completely unacceptable. Nobody should have to die like that.”
It is very unusual for MSF to launch large-scale lifesaving activities in well-resourced countries in Europe. But it also fits entirely with what MSF does worldwide – looking with a sharp focus for where the greatest vulnerability lies and trying to work out how best to help. The quadruple vulnerability in care homes – where people are elderly, frail, in need of care and living communally – has put them at the forefront of MSF’s struggle to respond to COVID-19.
Across Belgium, France, Italy, Portugal, Spain and Switzerland, MSF has advised or assisted in more than 300 care homes. More than 1,000 care home managers and staff have participated in webinars organised by MSF to share knowledge and experience about ways to continue providing the best care possible in ways that are safe and that maximise the effect of ‘shielding’ the residents.
“As a society, we will need to have a good think about why the priority in this pandemic has been hospitals and other medical facilities, and why barely a thought has been given to the most vulnerable,” says Dr di Lollo. “That will need to change.”
MSF will continue its approach of seeking out the most vulnerable groups of people and seeing how best to respond. Other projects in EU countries are addressing the needs of homeless people, asylum seekers and undocumented migrants, and prison detainees and guards. MSF teams are also preparing every project in the 70 countries where they work to be COVID-ready as the epidemic sweeps on around the globe, and has started caring for patients with COVID-19 disease in Africa, central Asia and Latin America. As in the EU, MSF teams will seek out the greatest need and the greatest vulnerability as the guiding principles of their response.
.jpg)
.jpg)
.jpg)